 May, 3 2026
May, 3 2026
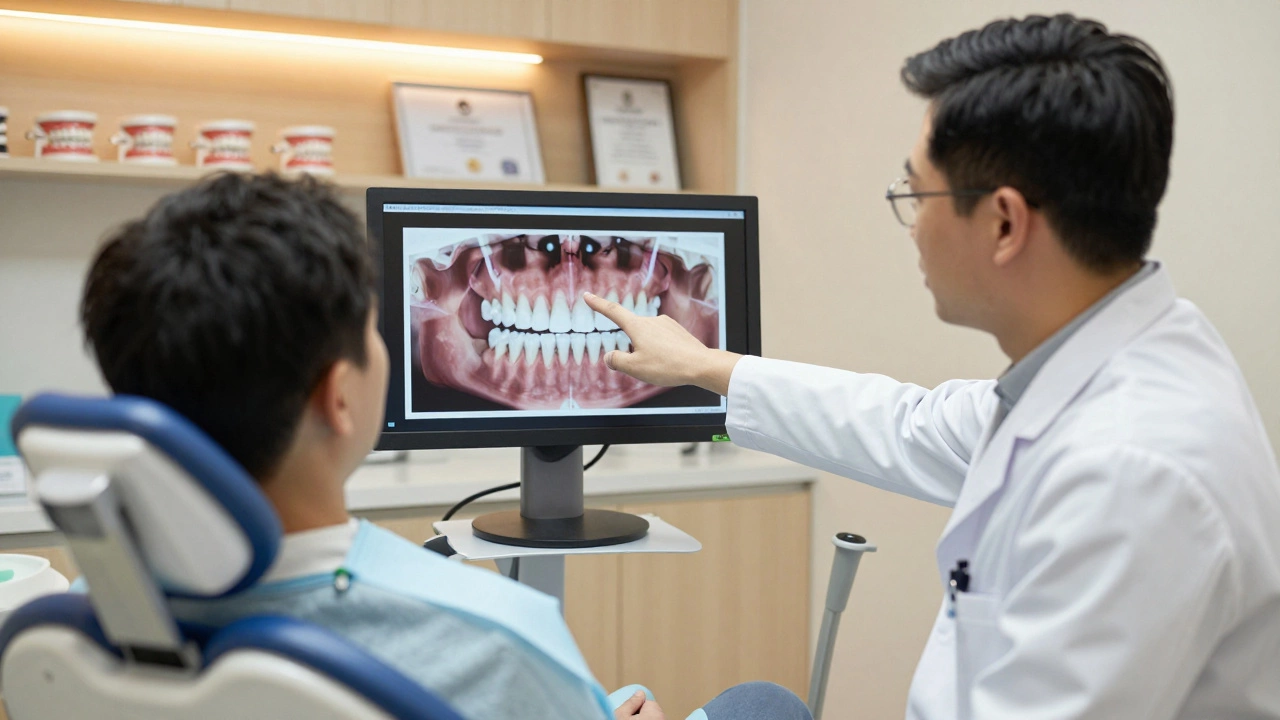
Dental Implant Eligibility Checker
Select Factors That Apply To You
Your Risk Profile
Risk Score
Select factors above and click "Assess" to see your personalized result.
Assessment Result
Recommended Next Steps:
If you are deemed ineligible for standard implants, consider discussing Dental Bridges, Partial/Full Dentures, or Resin-Bonded Bridges with your dentist. For severe bone loss, Overdentures anchored by fewer implants might still be viable.
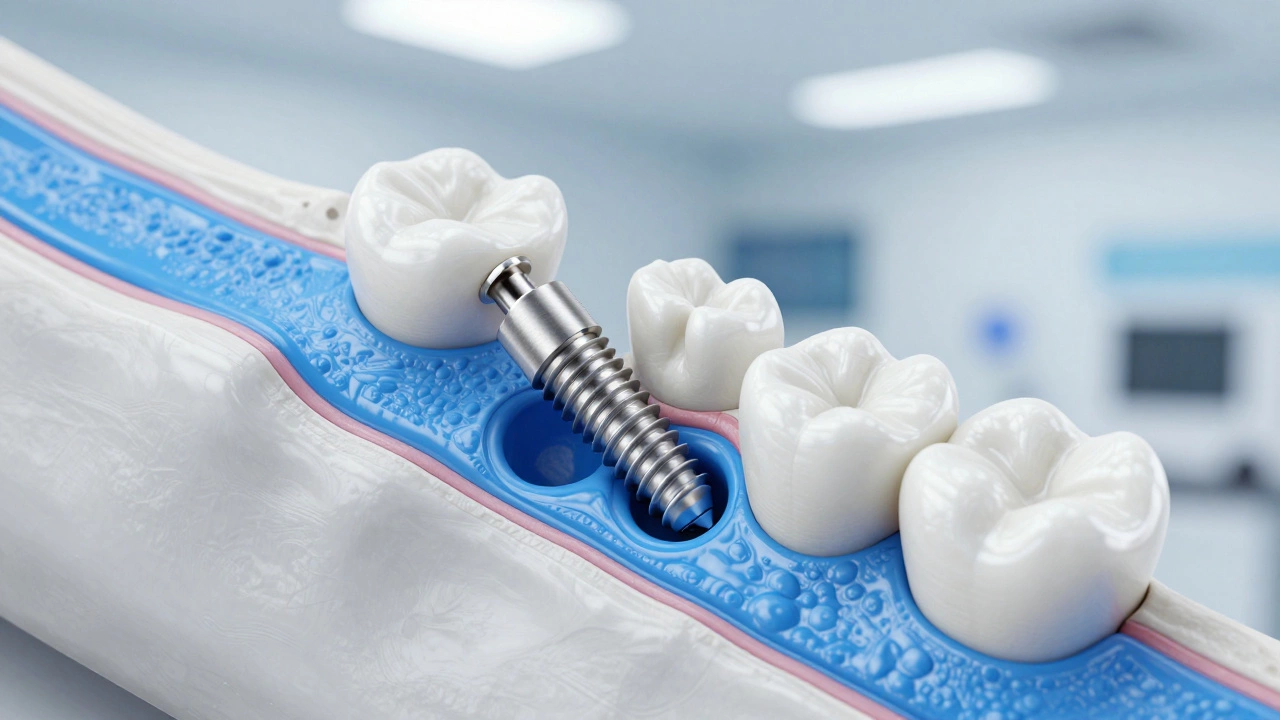
Wanting to replace missing teeth with dental implants is titanium posts surgically placed into the jawbone to support artificial teeth feels like a guaranteed fix. It isn’t. While success rates hover around 95-98% in healthy patients, certain health conditions, lifestyle habits, and anatomical factors can disqualify you from getting them-or at least make the procedure too risky without significant pre-treatment.
In the UK, where private dental care is the primary route for implants due to limited NHS coverage for state-funded healthcare services provided by the National Health Service, understanding your eligibility before booking a consultation saves time and money. This guide breaks down who cannot get implants, why specific conditions are barriers, and what alternatives exist if you’re told no.
Medical Conditions That Complicate Implant Success
Dental implants rely on a process called osseointegration, where the titanium post fuses with your jawbone. If your body struggles to heal or maintain bone density, this fusion fails. Several medical conditions directly interfere with this biological requirement.
Uncontrolled Diabetes is a major red flag. High blood sugar levels impair blood flow and slow down tissue healing. Studies show that patients with HbA1c levels above 8.0% have significantly higher rates of implant failure and infection. If you have diabetes, it must be well-managed and stable before a dentist will consider surgery. Your doctor may need to adjust medication timing around the surgical date to keep glucose levels optimal during healing.
Osteoporosis affects bone density, which is crucial for supporting an implant. While osteoporosis itself doesn’t automatically rule out implants, the medications used to treat it can cause problems. Bisphosphonates, drugs prescribed to prevent bone fractures, carry a rare but serious risk of osteonecrosis of the jaw (ONJ). This condition involves the death of bone tissue in the jaw, often triggered by invasive dental procedures. Patients taking high-dose intravenous bisphosphonates are generally considered ineligible for implants. Those on low-dose oral versions might still qualify after a thorough risk assessment by both their dentist and GP.
Autoimmune Diseases like rheumatoid arthritis or lupus can also pose challenges. These conditions often involve chronic inflammation and may require immunosuppressive drugs. Immunosuppressants weaken the body’s ability to fight off infections, increasing the risk of peri-implantitis-an inflammatory disease affecting the tissues around the implant. A specialist will evaluate whether your immune system is sufficiently active to handle the stress of surgery and subsequent healing.
Lifestyle Factors: Smoking and Oral Hygiene
Your daily habits play a huge role in whether you’re a candidate for implants. Two factors stand out as critical deal-breakers: smoking and poor oral hygiene.
Smoking is perhaps the most common reason people are denied implants. Nicotine constricts blood vessels, reducing blood flow to the gums and jawbone. This lack of circulation starves the healing site of oxygen and nutrients, drastically slowing recovery. Smokers are up to twice as likely to experience implant failure compared to non-smokers. In the UK, many private dentists refuse to treat current smokers entirely. Some may agree to proceed if you commit to quitting at least two weeks before and two months after surgery, but this requires strict adherence. Vaping is not yet fully understood in terms of implant outcomes, so most clinicians treat it with similar caution as traditional smoking.
Poor Oral Hygiene is another barrier. Implants don’t get cavities, but they can develop peri-implant disease, which mimics gum disease. If you struggle to keep your natural teeth clean, you’ll likely fail to maintain an implant. Dentists look for evidence of consistent brushing, flossing, and regular check-ups. If you have active gum disease (periodontitis), it must be treated and stabilized before any implant work begins. Placing an implant in an infected environment is a recipe for disaster.
Anatomical Limitations: Bone Loss and Sinus Issues
Even if you’re medically fit, your mouth’s structure might prevent implant placement. The most common issue is insufficient bone volume.
Bone Loss occurs naturally when teeth are missing. Without the stimulation from tooth roots, the jawbone resorbs (shrinks) over time. If there isn’t enough height or width in the jawbone, an implant has nothing to grip onto. In such cases, bone grafting surgery is required to rebuild the foundation. However, not everyone is a candidate for grafting. Severe bone loss, especially in the lower jaw near the inferior alveolar nerve, can make grafting too risky or impossible. Alternative solutions like overdentures or bridges might be suggested instead.
Sinus Problems affect upper jaw implants. The maxillary sinuses sit just above the upper back teeth. When these teeth are lost, the sinus cavity can expand downward, leaving little bone behind. If the sinus floor is too close to the intended implant site, the implant could protrude into the sinus, causing infection or chronic sinusitis. A sinus lift procedure can add bone, but again, this depends on individual anatomy and health. Chronic sinus infections themselves are a contraindication until resolved.
Medications That Interfere with Healing
Certain long-term medications can complicate implant therapy beyond just bisphosphonates.
Radiation Therapy to the head and neck region damages blood vessels and bone cells. Patients who have undergone radiation are at high risk for osteoradionecrosis, a severe condition where irradiated bone fails to heal. Implants are generally avoided in previously irradiated areas unless specialized hyperbaric oxygen therapy is used to enhance healing-a complex and expensive protocol.
Blood Thinners (anticoagulants) like warfarin or newer DOACs increase bleeding risk during surgery. They don’t necessarily disqualify you, but coordination with your cardiologist or GP is essential. Sometimes medication is paused briefly, or local hemostatic agents are used during surgery. Unmanaged bleeding risks can lead to hematoma formation, which compromises healing.
Immunosuppressants taken after organ transplants or for autoimmune conditions reduce infection-fighting capabilities. As mentioned earlier, this increases peri-implantitis risk. A multidisciplinary approach involving your transplant team or rheumatologist is necessary to weigh the benefits of replacing teeth against the risks of surgical intervention.
Psychological and Behavioral Considerations
Dental anxiety and unrealistic expectations can also influence eligibility. While not medical contraindications, these factors impact treatment success.
Severe Dental Anxiety or phobia may prevent you from cooperating during lengthy surgical procedures. Sedation dentistry options exist, but if anxiety is unmanageable even with sedation, alternative less-invasive treatments might be recommended. Trust and communication between patient and dentist are vital; if either is lacking, the outcome suffers.
Bruxism (teeth grinding) puts excessive force on implants. Unlike natural teeth, implants are fused rigidly to bone and lack the shock-absorbing periodontal ligament. Heavy grinding can loosen or fracture the implant components. If you grind your teeth, a night guard is mandatory. Failure to wear it consistently can void warranties and lead to early failure. Dentists assess bite forces carefully before proceeding.
| Factor | Impact on Implants | Potential Solution |
|---|---|---|
| Uncontrolled Diabetes | Slows healing, increases infection risk | Stabilize blood sugar levels first |
| Heavy Smoking | Reduces blood flow, doubles failure rate | Quit smoking 2+ weeks prior |
| Severe Bone Loss | No anchor point for implant | Bone grafting or alternative prosthetics |
| Bisphosphonate Use | Risk of osteonecrosis of the jaw | Avoid implants; consult oncologist/GP |
| Poor Oral Hygiene | High risk of peri-implantitis | Improve hygiene routine; treat gum disease |
NHS vs Private: Who Gets Covered?
In the UK, access to dental implants differs vastly depending on funding source. The National Health Service (NHS) covers essential dental treatments deemed clinically necessary rarely provides implants. They are typically reserved for exceptional clinical circumstances, such as:
- Patients who cannot wear conventional dentures due to physical disability or severe gag reflex.
- Congenital absence of teeth (hypodontia/anodontia) where functional restoration is critical.
- Post-cancer reconstruction where standard prosthetics are not viable.
For the vast majority of people seeking cosmetic or functional replacement of one or several teeth, implants are a private expense. This means you pay out-of-pocket, usually ranging from £1,500 to £3,000 per implant in the UK, excluding additional costs for bone grafts or crowns. Understanding your eligibility helps avoid paying for consultations that end in rejection.
Alternatives If You’re Not Eligible
If you fall into one of the ‘cannot’ categories, don’t lose hope. Modern dentistry offers robust alternatives.
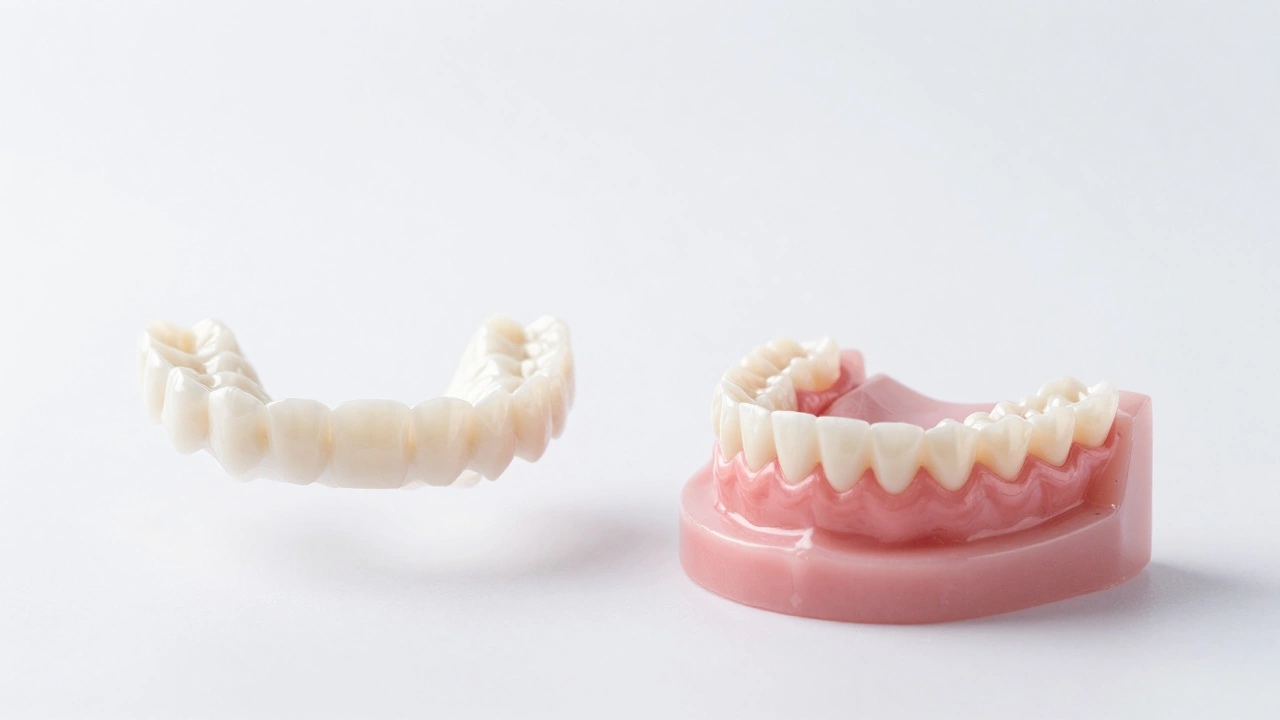
Dental Bridges use adjacent teeth as anchors to support false teeth. They don’t require surgery or bone integration, making them suitable for those with bone loss or medical restrictions. However, they involve shaving down healthy neighboring teeth.
Partial or Full Dentures are removable appliances. Recent advancements in flexible materials and precision fitting have improved comfort and aesthetics. For those with extreme bone loss, implant-supported overdentures (anchored by just 2-4 implants) might still be possible even if full arches aren’t.
Resin-Bonded Bridges (Maryland bridges) offer a minimally invasive option for replacing single front teeth, requiring little alteration to surrounding teeth.
Can I get dental implants if I smoke?
Most UK dentists will not place implants in current smokers due to high failure rates. You may be eligible if you quit smoking at least two weeks before surgery and remain abstinent for two months after. Consistency is key, as relapse significantly increases the risk of implant loss.
Does the NHS pay for dental implants?
The NHS rarely funds dental implants. They are only considered for exceptional clinical needs, such as inability to wear dentures due to disability or post-cancer reconstruction. For most patients, implants are a private, out-of-pocket expense.
What if I have osteoporosis?
Osteoporosis alone doesn't disqualify you, but medications like bisphosphonates can pose risks of osteonecrosis of the jaw. Your dentist will consult with your GP to assess risk. Low-dose oral bisphosphonates may allow for implants with careful monitoring, while high-dose IV users are typically excluded.
How much bone do I need for an implant?
Generally, you need at least 10mm of bone height and 6-7mm of width. If bone has resorbed due to long-term tooth loss, bone grafting may be needed. If grafting isn't feasible, alternatives like bridges or dentures are recommended.
Can diabetics get dental implants?
Yes, but only if diabetes is well-controlled. An HbA1c level below 8.0% is typically required. Poorly controlled diabetes impairs healing and increases infection risk, leading to higher failure rates. Coordination with your endocrinologist is essential.
